Running Injuries can usually be successfully treated by a combination of manual therapies followed by specific rehabilitation exercises to prevent recurrence of the injury.
Solutions 4 Sports Injuries
Running Injuries can usually be successfully treated by a combination of manual therapies followed by specific rehabilitation exercises to prevent recurrence of the injury.
Page Menu
- Iliotibial Band Syndrome
- Achilles Tendonopathy
- Shin Splints
- Stress Fractures
- Muscle Strain
- Runners Knee
- Plantar Fasciitis
Sports Injuries Advice
"The general advice I give to those that have suffered a recent injury is firstly to apply the RICE rule which is to Rest (stop exercising), Ice (the area of swelling), Compression (apply a compressive bandage or support to the area that is swollen), and to Elevate (raise the leg slightly when sitting or lying to allow drainage of the fluid)".
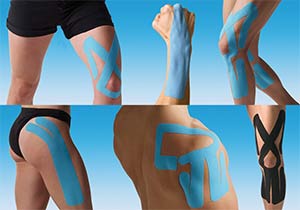
"Firstly, I take a thorough history and perform an examination of the involved area(s) to determine the cause and type of injury that has occurred. Depending on the type of sports injury I use a selection of manual therapies to treat it. These may include chiropractic mobilisation/manipulation of the joint including the spine if implicated, deep/soft tissue massage and trigger point therapy to involved muscles to help relax the tension and reduce spasm, ultrasound to reduce swelling and inflammation of ligaments and tendons, kinesiotaping to provide support to the area and to help drain fluid from the injury site, dry needling (medical acupuncture) to involved muscles and ligaments to reduce tension and remove any trigger points from the muscle."
"I would also check for any spinal alignment issues that may be connected to the injury as well as check general posture and pronation/supination of the foot arch. I would also check the condition of the running shoe. The aim is to identify the potential cause of the injury if no trauma was involved."
"Once the injury is in its recovery phase I would then provide specific stretches and strengthening exercises to rehabilitate the weakened area, which will also reduce the risk of recurrence of the injury."
The most common running injuries
Generally speaking the healing time for the ligaments, tendons and muscles involved in running injuries is 6 weeks. During this time it may be that resting is advised whilst the injury is going through the healing process. Other options for exercise may include cross training techniques such as swimming, cycling and using the gym as well as doing all the rehabilitation exercises suggested for the specific injury.
Iliotibial Band Syndrome (ITBS)
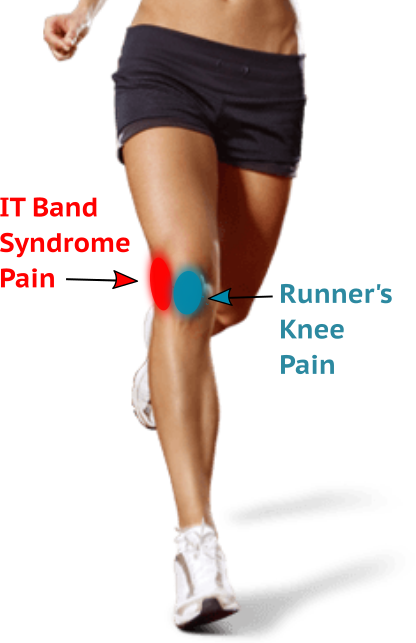
The iliotibial band (ITB) is a thick, fibrous band that runs along the outside of the thigh from the hip to the tibia passing along the outside of the knee joint. During running the knee will flex and extend repetitively causing the ITB to rub on the femur (thigh bone). As it crosses the outside of the knee the ITB gets impinged causing irritation and inflammation. This commonly occurs if you increase your mileage too quickly or if you do a lot of downhill running or speed work. It can also occur if you always run on the same side of the road as it puts a lot of stress onto the side of the knee. Runners who over-pronate or have weak gluteal and hip abductor muscles are also at risk as this causes uncontrolled hip motion resulting in an overstretch of the ITB resulting in irritation.
Treatment
Reduce the inflammation by using ice, resting and reduce your mileage. Cross training such as swimming, pool-run or using a cross trainer can be useful at this stage. Once the inflammation is under control treating the ITB and TFL, quadriceps and hamstrings with techniques such as deep tissue massage and using a foam roller to reduce the tension in these muscles. Specific stretching of the tightened muscles and strengthening of the weak muscle groups such as the gluteals and hip abductors will help to stabilise the hip. Address any pronation of the feet by having a gait analysis by your local running shop or seek professional help e.g. a podiatrist or orthotics
Continuing with the exercises, foam rolling and using ice post run is a good way of preventing recurrence of the injury. Also varying your running routes and type of training so that you limit how often you train on the track or hills.
Achilles Tendinopathy (tendinitis)
The Achilles tendon attaches the calf muscles (gastrocnemius) to the back of the heel (calcaneus). Under excessive stress the tendon tightens which is often felt as a stiffness of the tendon, it then becomes irritated and inflamed (tendinitis). This is often felt as a burning type pain and swelling close to the back of the heel which can be sharp. Unfortunately, due to reduced blood supply to the tendon it is usually slow to heal.
Runners who over-pronate are often at risk of this injury but it can occur through wearing poor and unsupportive footwear (i.e. old running shoes). Other causes include increasing the intensity of training too quickly i.e. hill and speed training without building up slowly as well as increasing the mileage too quickly. This results in the tightening of the calf muscles resulting in the tightening of the Achilles.
Treatment
Reduce the inflammation and swelling by using ice regularly and resting. Cross training such as swimming can be useful through this phase. As the inflammation reduces seeking treatment such as deep tissue massage for the calf muscles and cross friction techniques for the Achilles tendon will start to loosen the tightness. This can be followed by gentle calf stretches to increase the ankle flexibility. Addressing any pronation by having a gait analysis by your local running shop or visiting a podiatrist to discuss the use of orthotics. Strengthening any weakened muscles such as the gluteals and hip abductors as well as the calf muscles and specific exercises (heel drops) to lengthen the Achilles tendon. Once your injury allows you to return to running it is best to slowly increase your mileage and to avoid overtraining on the hills and track or speed-work.
Continuing your exercises, using ice post run and keeping your calf muscles strong will prevent recurrence of this injury and also if you over-pronate you always wear shoes with an arch support.
Shin Splints
"Shin splints" or medial tibial stress syndrome occurs in 30-40% of new runners and can occur in those returning to running after a long rest period. It is usually a sign of "too much too quickly" or too much running on hard surfaces. It can also be related to wearing old worn out running shoes, and can affect runners with over pronation or with high arches. Some believe that it can also be caused by over striding forcing the shin to absorb the shock. It often starts as an ache in front of the shin that results in small tears in the muscles (tibialis anterior) attached to the tibia (shin bone). In severe cases shin splints can result in a stress fracture.
Treatment
The initial approach is to rest, ice and ease up on your mileage and avoid running on hard surfaces. Running on softer surfaces e.g. grass to reduce impact on the shin and make sure you stop wearing old worn out shoes. Seeking professional help and having treatment on the muscles to clear the trigger points by deep tissue massage and/or dry needling followed by specific rehabilitation to stretch and strengthen all of the lower limb including the shin muscles as well as calf, hip and core muscles.
When recovered and to avoid a recurrence of the injury begin by slowly increasing your mileage, mix running on hard and softer surfaces to reduce impact on the shin and continue with the rehabilitation exercises. Also change your shoes every 300 miles or as recommended.
Stress Fractures
Stress fractures are one of the most serious runner's injuries and usually develop as a result of overtraining. The common sites are the shin (tibia), feet (metatarsals or calcaneus), ankle (distal end of the fibula). They are usually characterised by pain running as well as pain felt by just being on your feet and moving around. Often the pain is localised to a specific point when touched. Diagnosis is confirmed by X-Ray.
If in doubt about your injury contact your GP.
Muscle Strain
Runners can suffer from strains to their leg muscles including the hamstrings (the large muscle that runs down the back of the leg to the knee), the calf muscles (the muscle that runs from the back of the knee to the Achilles tendon/heel) and the quadriceps (the muscle that runs down the front of the leg to the knee). The cause is usually due to tightness in the muscle or from muscle imbalance and weakness. Often the pain is acute as it comes on suddenly and strong resulting in bruising from the tear within the muscle.
Treatment
Rest and ice helps to reduce inflammation and swelling and the use of arnica will draw any bruising out of the muscle. When the swelling and inflammation have improved, professional treatment may include soft tissue massage or foam rolling, kinesio-taping and dry needling of the muscle. Gentle stretching of the involved muscle and cross training such as swimming and pool running are good activities. As symptoms improve strengthening the muscle as well as looking at any muscle imbalance will help to avoid recurrence of the injury. Consider including exercises for the hips to improve stabilisation.
Continuing with the stretch and strength programme and gradually introduce any hill or speed training. Avoid too much of this type of training so as not to overload the muscles. Consider wearing compression tights/socks as these help with blood flow to the muscles.
Runner's Knee or Patellofemoral pain syndrome (PFPS)
Approximately 40% of running injuries are knee injuries. PFPS is usually characterised by a constant ache underneath the kneecap (patella) that worsens as the intensity of the exercise increases. It typically flares up during or after a long run, after extended periods of sitting or while descending hills and stairs. The cause is due to irritation of the cartilage on the underside of the kneecap that can be aggravated by running on uneven surfaces, muscle imbalance particularly due to weakness of the gluteal muscles and hip abductors or it is due to the improper tracking of the patella during running. It can also be caused by running in poor shoes and those with over-pronation are also at risk.
Treatment
Seeking professional help to assist in the realignment of the patella tracking through the use of taping techniques can help aid recovery. Identifying over-pronation as a possible cause through a gait analysis and the prescription of the correct running shoe or orthotics. Rehabilitation to correct muscle imbalance including the quadriceps, hamstrings, gluteal muscles and hip abductors. Resting by cross training including cycling to improve muscle strength is a good activity. Once recovered a gradual return to running – 'pain-free' is advised.
Plantar Fasciitis
One of the most common foot injuries. The plantar fascia is he long ligament that runs from the heel along the sole of the foot. Plantar fasciitis is micro-tearing or inflammation/irritation of the fascia usually where it attaches to the heel. It is characterised by a sharp pain in the heel or arch of the foot during the first few steps from getting out of bed or after a prolonged time sitting that eases as you move around. There are several causes including poor running shoes, wearing shoes without sufficient arch support, long periods of standing or walking on hard surfaces without supportive footwear as well as overtraining. Tightness of the calf muscle and hamstrings or weakness of the gluteal muscles and also a history of low back pain can also contribute due to the change in the normal walking pattern.
Treatment
Complete rest from running is usually recommended as continually running can delay healing. Recovery time can be 3-12 months depending on the approach taken but 6 months is often quite common. Cross training such as cycling and swimming are good activities. Regular icing using a frozen water bottle and rolling the foot for 5-10 minutes regularly through the day helps reduce the inflammation. Taping techniques help to support the arch. Using a golf ball and rolling the foot for 10 minutes regularly helps to stretch the tendon as well as stretching the foot by gently pulling the toes back. Also stretching the calf and hamstrings and using a foam roller to reduce tightness of these muscles. Addressing muscle imbalance such as strengthening the core muscles help to strengthen the lower back and also strengthening of the gluteal and hip muscles to stabilise the pelvis. Wearing supportive shoes and possibly seeking professional help for orthotics or making sure you are wearing the correct style of shoe for your foot type.
Continuing with your rehabilitation routine will help avoid recurrence of the injury and making sure that you always wear shoes with arch supports.

